TMJ Total Joint Replacement Surgery
When other treatments haven’t worked, total joint replacement can restore the jaw function and quality of life you’ve been missing.
TMJ / TMJ Arthrocentesis / Jaw Corrective Surgery
You’ve Been Through a Lot to Get Here
If you’re reading this page, you’ve likely been dealing with severe jaw pain and dysfunction for a long time. You may have already tried splints, medications, physical therapy, arthrocentesis, or even previous jaw surgeries — and you’re still suffering.
That’s not unusual. TMJ total joint replacement is reserved for patients with end-stage temporomandibular joint disease — meaning the joint itself is too damaged to be preserved. You’re not here because you didn’t try hard enough. You’re here because your condition requires a definitive solution.
You may be a candidate if you experience:
- Severe, persistent jaw pain that limits your daily life
- Significant difficulty opening your mouth, chewing, or speaking
- A diagnosis of advanced degenerative joint disease, ankylosis, or avascular necrosis
- Failed results from previous TMJ treatments or surgeries
- Joint damage from autoimmune conditions such as rheumatoid or psoriatic arthritis
- Structural destruction from trauma or tumor resection
What we want you to know: This is one of the most impactful procedures in oral and maxillofacial surgery. Patients who have struggled for years — sometimes decades — consistently report significant improvements in pain, function, and overall quality of life after total joint replacement.
Your Journey — Step by Step
We walk you through every stage so you know exactly what to expect — from your first visit to full recovery.
Consultation and Evaluation
Your first visit is a thorough assessment — not a sales pitch. We’ll review your full history, examine your jaw, and take CT imaging to evaluate the condition of your joint in detail. If you’ve had previous surgeries, we’ll want to review those records too.
We’ll explain all of your options honestly. If a less invasive treatment could still help, we’ll tell you. Total joint replacement is only recommended when it’s genuinely the best path forward.
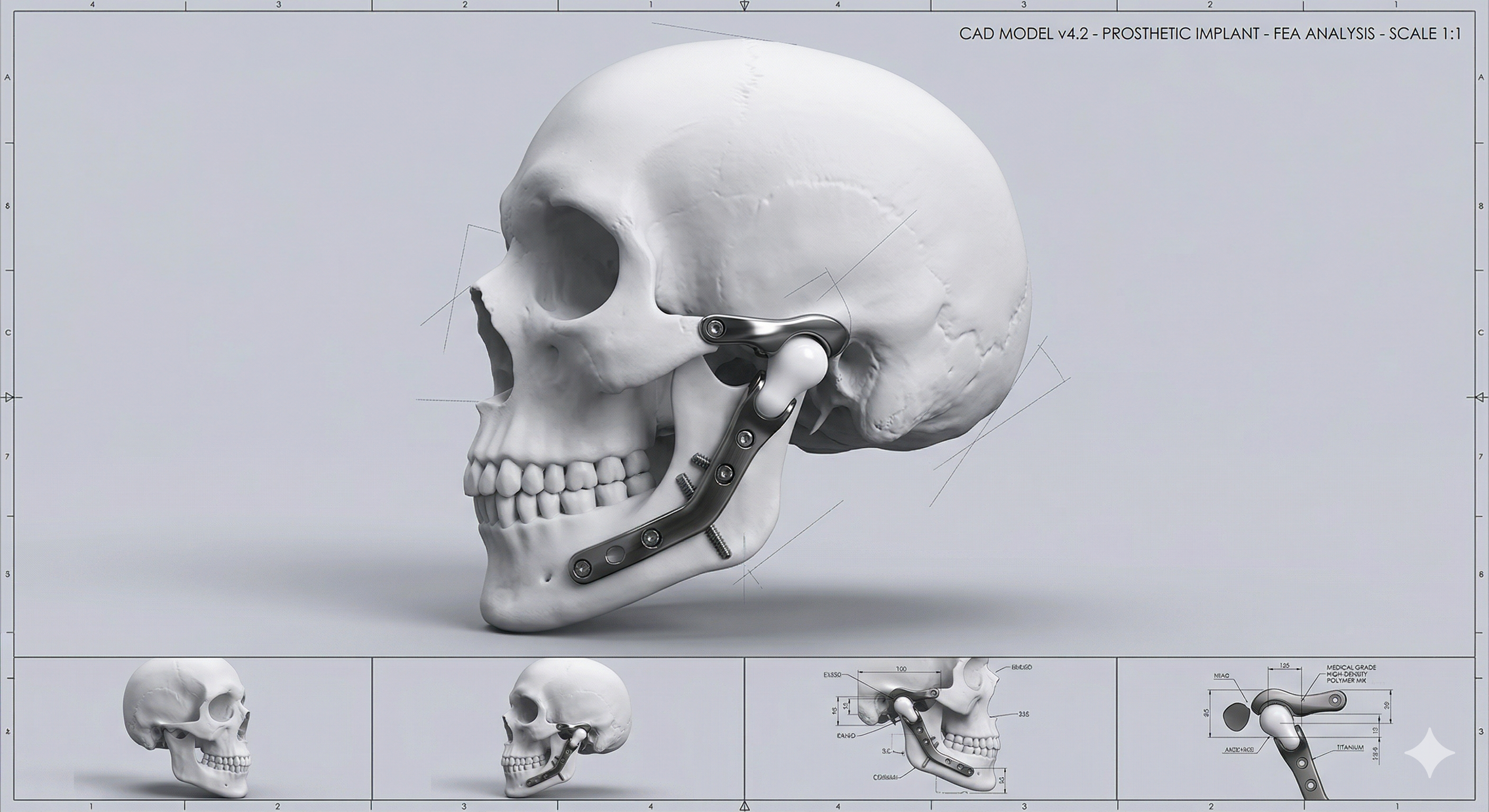
Custom Prosthesis Design
This is not an off-the-shelf implant. Your prosthesis is custom-designed and manufactured to fit your specific anatomy. Using your CT scans, a 3D model of your jaw is created, and the prosthetic components — a fossa component (attached to the skull base) and a condylar component (attached to the lower jaw) — are engineered to match.
Before manufacturing, our team reviews and approves the virtual surgical plan to ensure precision.
The Day of Surgery
Surgery is performed under general anesthesia at a hospital — not in an office setting. Through carefully planned incisions near the ear and beneath the jaw, the damaged joint is removed and replaced with your custom prosthetic components.
In many cases, a fat graft is placed around the new joint — a well-established technique that significantly reduces the risk of scar tissue formation. The procedure typically takes 3 to 5 hours, depending on complexity and whether one or both sides are treated.
Hospital Stay
Most patients stay in the hospital for 1 to 3 nights. The surgical team monitors your recovery, manages your comfort, and ensures everything is healing as expected. Your jaw may be supported with light elastic bands to guide your bite into proper alignment.
Recovery at Home
Week 1: Rest is the priority. You’ll be on a liquid and non-chewing diet — smoothies, soups, protein shakes, yogurt. Swelling and stiffness are normal. Cold compresses and prescribed medications help manage discomfort.
Weeks 2–6: Transition to very soft foods. Once cleared, you’ll begin gentle jaw exercises — opening, side-to-side movements, and protrusion — done in short sessions, multiple times per day, to prevent stiffness.
Weeks 6–12: Gradual return to a normal diet and regular activities. Some patients work with a physical therapist during this period to optimize their recovery.
3–6 Months and Beyond: Continued improvement in function and comfort. The prosthetic joint is designed for long-term durability — published data shows strong outcomes at 20+ years.
A note on weight: It’s common for patients to lose 10 or more pounds during the initial recovery period due to the soft diet. This weight typically returns once normal eating resumes. We recommend high-protein nutrition shakes to maintain calorie intake during the early weeks.
Why MONT Surgery
Dr. Maryam Farag
Dr. Farag has developed a particular clinical focus in the diagnosis and surgical management of TMJ disorders. She serves as an Assistant Attending Oral and Maxillofacial Surgeon and Clinical Instructor in Surgery at NewYork-Presbyterian/Weill Cornell Medicine, where she manages complex TMJ pathology as part of a multidisciplinary hospital-based team.
Dr. Jay D. Kim
Dr. Kim completed a six-year residency at NewYork-Presbyterian/Weill Cornell that included extensive TMJ surgery training. He holds both a medical and dental degree — providing a deeper understanding of the anatomy, physiology, and systemic considerations involved in complex jaw surgery. He has over 15 years of clinical experience.
Academic-Caliber Care, Private Practice Attention
Both surgeons maintain active hospital and university appointments at NewYork-Presbyterian Hospital, Weill Cornell Medical College — one of the nation’s leading academic medical centers. You receive the precision and rigor of an academic surgical center, with the personal attention that comes from a surgeon-owned practice.
Custom Technology, Not Compromises
Every TMJ total joint replacement at MONT begins with CT imaging and 3D virtual surgical planning. Your prosthesis is designed from your anatomy — not adapted from a generic template. The surgical suites are equipped with the latest imaging and instrumentation to ensure precision at every step.
Benefits
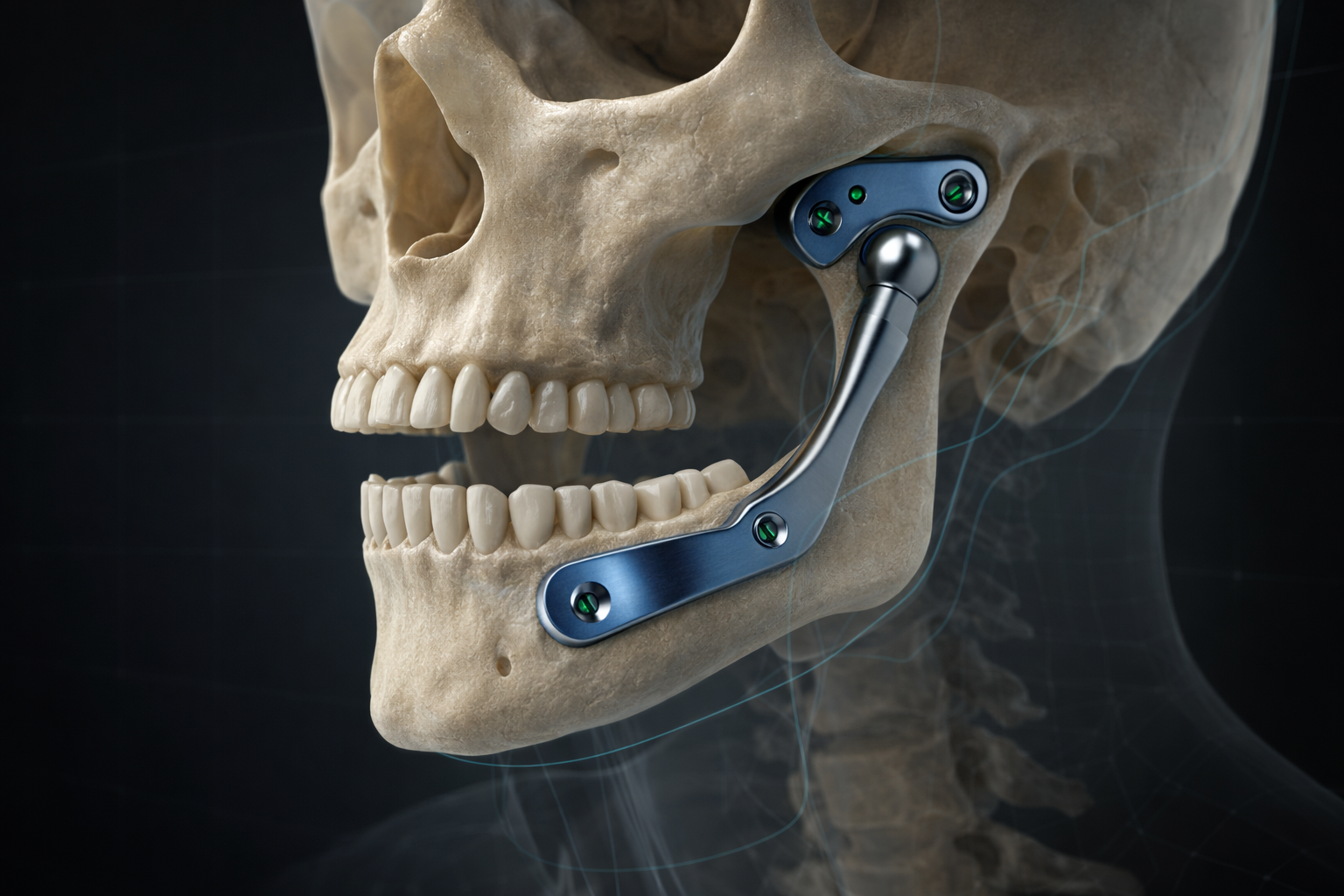
- Custom prosthesis designed from CT imaging to fit your unique anatomy
- Restores jaw function in end-stage joint disease when other treatments have failed
- Significant, lasting reduction in chronic TMJ pain
- Long-lasting prosthetic joint system with strong published outcomes at 20+ years
- Performed at a hospital under general anesthesia for maximum safety
- Fat grafting technique reduces risk of post-surgical complications
- Coordinated care between experienced surgeons and referring specialists
Frequently Asked Questions
Total joint replacement is considered when the joint itself is too damaged to be preserved — typically due to severe degenerative disease, ankylosis, or failed previous surgeries. During your consultation, we’ll evaluate your specific situation with CT imaging and a thorough clinical exam. If a less invasive approach like arthrocentesis could still help, we’ll recommend that first.
Take the Next Step Toward Relief
If you’ve been living with chronic jaw pain and previous treatments haven’t given you relief, we’re here to help. Schedule a consultation to discuss whether TMJ total joint replacement is right for you.
Request AppointmentPatient Testimonials
Dr. Farag was incredible with my TMJ treatment. She really listened to my concerns and developed a personalized treatment plan.
Verified Patient — TMJ
